Upper airway resistance syndrome (UARS) is a condition that was first identified and described at Stanford University. Like obstructive sleep apnea (OSA) or (OSAHS), UARS results in the soft tissue of the throat relaxing and a reduction in the size of the airway-the main difference being that apneas (pauses in breathing) and hypopneas (decreasing in breathing) are absent or very low in patients with UARS. Patients with UARS require a greater effort in breathing to get past the narrowing or obstruction in their airways. The brain has to arouse itself from deeper stages of sleep to increase respiratory efforts.
The EEG arousals from sleep that UARS causes are called respiratory effort-related arousals” (RERAs). These RERAs are often undetected by the affected individual. When this scenario repeats throughout the night, sleep is impaired, just like in obstructive sleep apnea. However with UARS there is no obvious oxygen desaturation like with OSA, this often makes UARS difficult to detect.
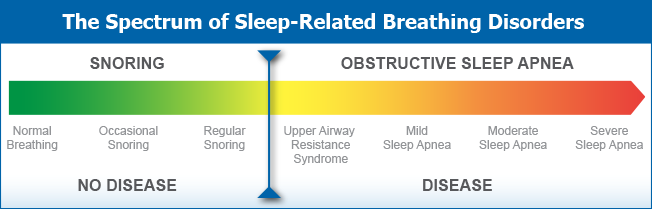
UARS is best described on the spectrum as the progression from snoring towards OSA. However, the presentation of UARS is unique. Unlike OSA or OSAHS, UARS presents in women and men equally and can be found more in thin or normal body structured individuals.
The manifestations of UARS are varied but the most common symptoms are:
- Disturbed sleep with consequent daytime impairment, including excessive daytime sleepiness and frequent arousals from sleep
- Morning headaches
- Decreased concentration
- Headaches
- Difficulty with sleep onset and sleep maintenance (insomnia)
Recent research continues to recognize that the clinical features seen in UARS overlap with functional somatic syndromes such as chronic fatigue syndrome, fibromyalgia, irritable bowel syndrome (IBS), and chronic headache.
Even more recent, is the research linking temporomandibular joint (TMJ) syndrome to an underlying sleep problem, particularly UARS. It is also important to note, snoring is not a necessary feature of this syndrome.

As mentioned, UARS represents a progression of disease bridging the transition from “benign snoring” to obstructive sleep apnea. Patients simply do not go to bed normal one night, only to awaken the next morning with obstructive sleep apnea. Instead, they typically go through natural progression over time or following weight gain from “benign snoring”, to UARS, and finally to obstructive sleep apnea. This progression may take years or decades to occur.
Diagnosis
Diagnosis of UARS requires symptoms (excessive daytime somnolence, frag- mented sleep, fatigue), anatomic features consistent with upper airway narrowing, and supportive PSG findings. The measurement of esophageal pressure is the gold standard for measuring respiratory effort and is the only consistent measurement reported for the diagnosis of UARS. Although these diagnostic measures must be ordered by a physician and read by a sleep doctor for a diagnosis, often it is a dentist who first notices signs and symptoms and screens for sleep disorders such as UARS. This is because of the relationship between the airway and facial and jaw development. At MHHC Sleep Solutions we can perform comprehensive airway evaluation with pulse oximeter screening if necessary to help your doctor identify any sleep disordered breathing disorders such as UARS that maybe impacting your life.
Treatment
Treatment for UARS is often similar to the treatments of OSA. However CPAP therapy maybe the last resort treatment option for UARS as compared to the “go-to” option for those suffering from severe OSA. It is important to talk to your sleep doctor about treatment options if you are diagnosed with UARS. Options often include:
Behavior and Lifestyle treatments-This may include practicing good sleep hygiene and making sleep a priority, getting adequate exercise, avoiding blue light and caffeine and or alcohol before bedtime, changing positions of sleep. Nasal cones and or mouth taping maybe an important step to decrease nasal resistance and improve oxygen levels in the body.
Oral Appliances– Dental appliances are often the first option for treating UARS. An oral sleep appliance is worn in the mouth only while you sleep and fits like a sports mouth guard or an orthodontic retainer. Oral appliances support your jaw in a forward position to keep the oral airway open. Oral appliances are quiet, portable and easy to care for. In 1995, the Task Force for the Standards of Practice Committee of the American Sleep Disorders Association recommended offering oral appliances to all non-apneic snorers. At MHHC Sleep Solutions we can provide you with a sleep oral appliance that is effective and comfortable. Talk to us more about oral appliance options.
Surgery– Nasal airway anatomic issues such as a deviated septum, inferior turbinate hypertrophy, nasal valve collapse, or any combination, have been associated with UARS and may need to be evaluated.
At MHHC Sleep Solutions, we believe that it is important to identify patients with UARS, not only because of the health risks associated with UARS, but especially because they may have a particularly higher risk of developing obstructive sleep apnea in the future. An important reason to treat UARS is to allow the patient to obtain a better quality of sleep. Opening the airway or decreasing the upper airway resistance can reduce the number of arousals during sleep, improve the ability to initiate or maintain sleep, lead to more refreshing sleep, and improve daytime alertness. Contact us today to learn more about UARS or if an oral appliance or other dental treatment options can benefit you if you have been diagnosed with UARS.
